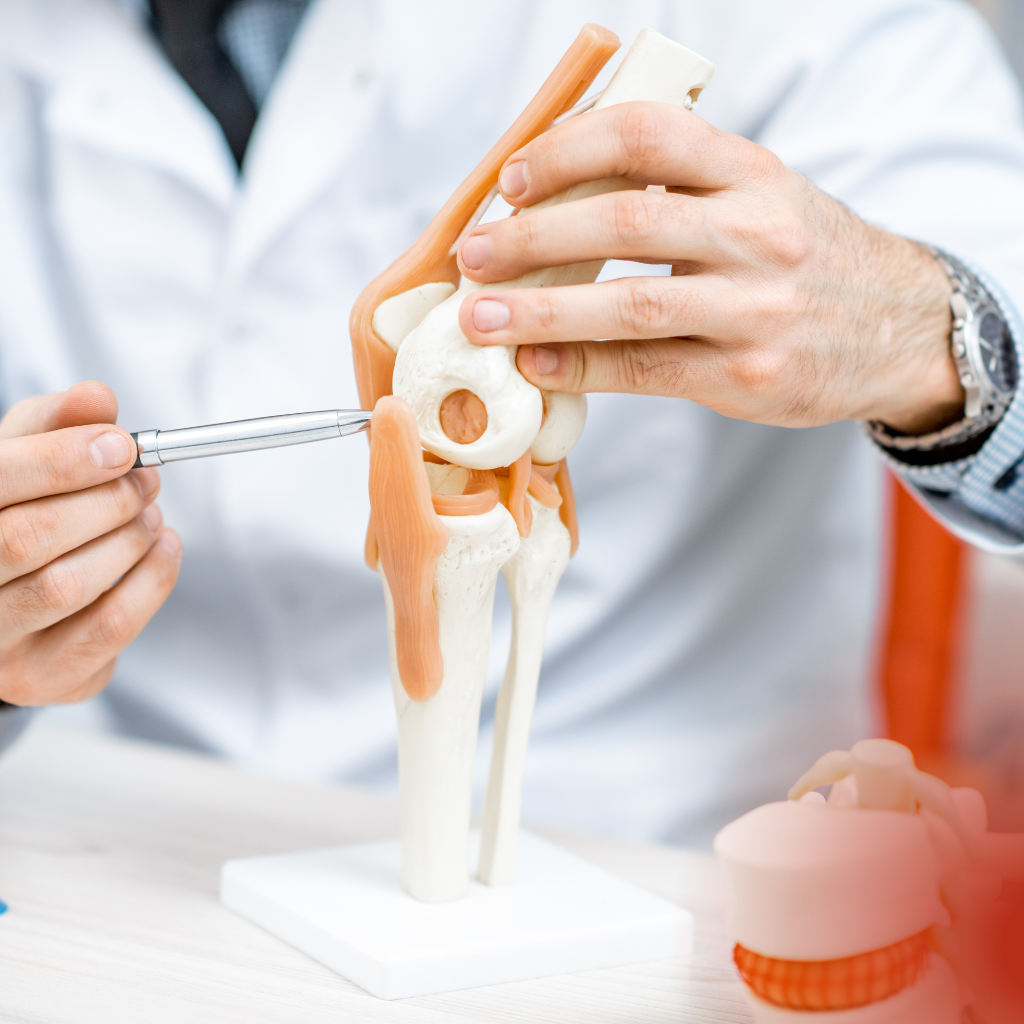
Arthroplasty, also known as joint replacement or joint prosthesis surgery, refers to the surgical procedure where a damaged joint is replaced with an artificial joint made from metal, ceramic, or plastic. In most cases, the entire joint is replaced, but in some rare instances, only the damaged part of the joint may be substituted. The most commonly replaced joints are the hip, knee, and shoulder.
What is Arthroplasty?
Arthroplasty is the medical term for joint replacement surgery. During the procedure, the orthopedic surgeon removes the damaged joint and replaces it with an artificial one, known as a prosthesis, which can be made of metal, ceramic, or durable plastic. The new joint looks and functions similarly to a natural one. Although joint replacements can be performed on any joint in the body, the most common types are hip and knee replacements. Most people who undergo arthroplasty require a total joint replacement, while partial joint replacement is suitable for only a small number of patients. This involves replacing just the damaged section of the joint.
Recovery After Arthroplasty
Recovery time varies from person to person and depends on factors such as age, pain level, lifestyle, the type of procedure, and the specific joint that was replaced.
Who Needs Arthroplasty?
Orthopedic surgeons may recommend arthroplasty in the following situations:
- Persistent joint pain that does not improve with non-surgical treatments like physical therapy, medications, injections, assistive devices, or rest.
- Joint stiffness and limited mobility that hinder or make daily activities impossible.
- Swelling and inflammation that do not improve with medication or lifestyle changes.
These symptoms may stem from various conditions, including:
- Arthritis, particularly osteoarthritis.
- Rheumatoid arthritis.
- Fractures, such as a hip fracture.
- Joint abnormalities, like hip dysplasia.
- Avascular necrosis, where bone tissue dies due to a lack of blood supply.
Which Joints Can Be Replaced?
Surgeons most commonly replace the hip and knee joints, referred to as hip arthroplasty and total knee replacement, respectively. In the U.S., approximately 500,000 total hip replacements and over 850,000 total knee replacements are performed annually. Today, surgeons can replace the following joints:
- Hips
- Knees
- Elbows
- Wrists
- Shoulders
- Toes
Preparing for Arthroplasty
Your doctor will help you prepare for the procedure. In the weeks leading up to surgery, they may recommend physical therapy, exercises, or dietary changes to ensure you are in optimal health. You may need blood and urine tests, an electrocardiogram, and chest X-rays to assess your overall health. Depending on your medical history, consultations with specialists in anesthesia, cardiology, or internal medicine may be required. Imaging tests like CT scans or MRIs may also be necessary to aid surgical planning. Be sure to inform your doctor about your medical history and any medications you are taking, as some medications (such as blood thinners) may need to be stopped before surgery. Additionally, your doctor will advise you when to stop eating and drinking the night before the procedure.
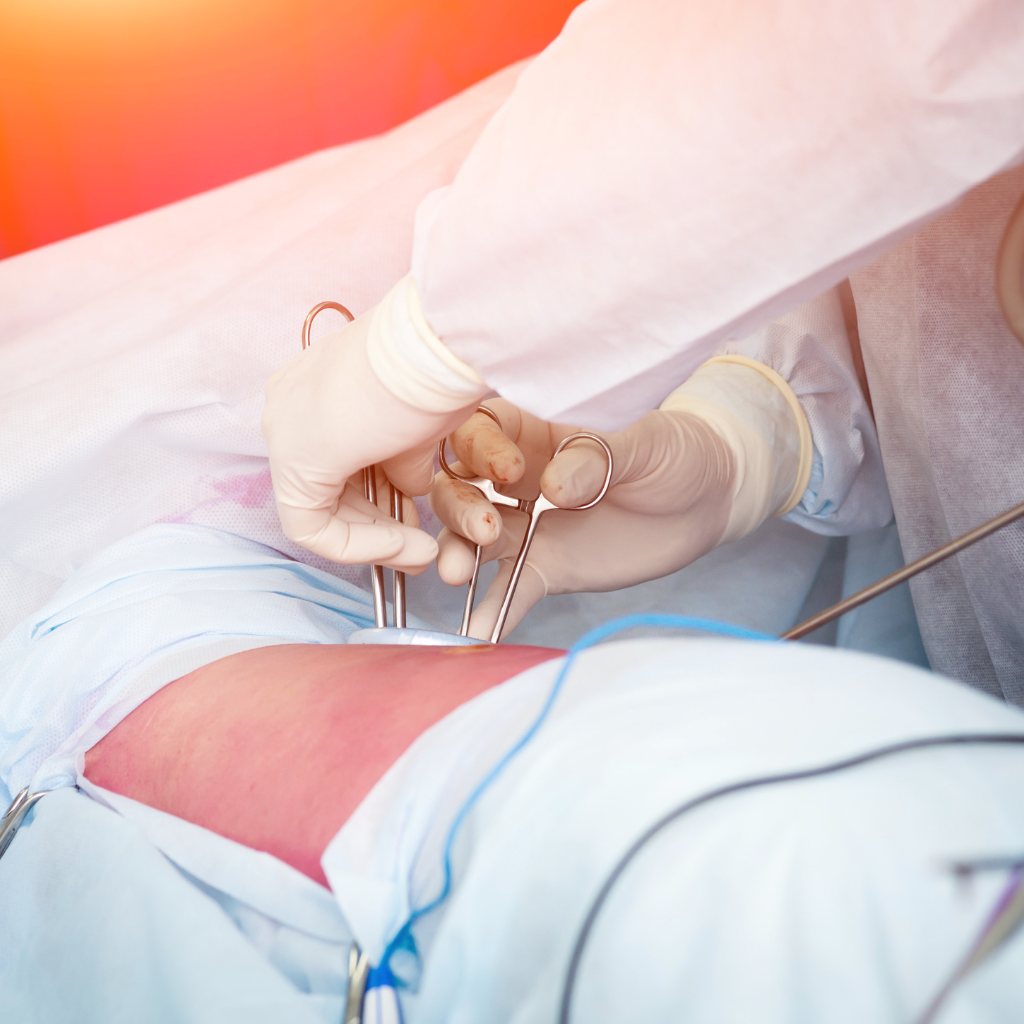
How is Arthroplasty Performed?
You will undergo the surgery in a fully equipped hospital. The specific technique used will depend on the type of surgery and the joint being replaced. Just before the procedure begins, anesthesia is administered to prevent pain. The orthopedic surgeon will make an incision to access the damaged joint, remove it, and replace it with an artificial joint. The incisions will then be closed with stitches, staples, or surgical glue. Bandages will be applied, and in some cases, you may need a brace or sling for support. Some joint replacement surgeries can be performed using minimally invasive techniques, which involve smaller incisions and specialized instruments, leading to shorter recovery times. Your orthopedic surgeon will recommend the most suitable approach for you.
What to Expect After Arthroplasty
Depending on the type of procedure, you may go home on the same day or stay in the hospital for one or two days. Your doctor will guide you through the recovery process. You will need someone to drive you home after surgery and may require assistance with daily tasks such as using the bathroom, eating, or bathing. It is normal to experience some pain in the first few days after surgery. During this period:
- Avoid strenuous activities. Focus on rest to support the healing process. Your doctor may suggest applying ice packs or cold compresses to the new joint for 20-minute intervals.
- Follow your physical therapy and home exercise program. Adhering to these instructions is essential for restoring joint function and protecting the new joint.
- Elevate the joint. Depending on the joint involved, your doctor may advise keeping it elevated while resting. For example, if you had knee surgery, you can rest your foot on a stool or chair.
- Keep the surgical site clean and covered. Follow your doctor’s wound care instructions carefully and ask when you can remove the dressing or take a shower.
- Take pain medications as directed. Your doctor may recommend over-the-counter NSAIDs or prescription pain relievers. Additionally, some medications may be necessary to reduce swelling or prevent blood clots.
Benefits of Arthroplasty
Joint replacement procedures allow people to move without pain or stiffness. After surgery, many patients can resume activities they once enjoyed, leading to an improved quality of life and better overall health.
Risks of Arthroplasty
Like any surgery, arthroplasty carries risks, including:
- Blood clots
- Infection
- Nerve injury or damage around the joint
- Fracture due to joint stiffness, weakness, or instability
- Dislocation or other issues with the new joint
Certain medical conditions, such as diabetes, hemophilia, or autoimmune diseases like lupus, can increase the risk of complications. It is important to inform your doctor of these conditions beforehand, as they can make recovery more challenging.
When Can You Resume Normal Activities?
Everyone’s recovery timeline is unique. Talk to your doctor about when you can return to activities you enjoy. It is helpful to have this conversation before surgery to set realistic expectations about which activities will be suitable for you after full recovery.
What Affects Recovery Time?
Several factors can influence your recovery time, including:
- Activity level and lifestyle
- Age
- Which joint was replaced
- Presence of other health conditions or orthopedic problems
- Whether the procedure was a total or partial joint replacement
Following a proper physical therapy program can accelerate recovery. Physical therapy strengthens the muscles around the new joint, providing better support, enhancing flexibility, and improving mobility.
How Long Do Artificial Joints Last?
The lifespan of a joint replacement typically ranges from 10 to 15 years, though individual outcomes may vary. Talk to your doctor about how to care for your new joint. If the prosthesis wears out after 15 years, it can be replaced with a new one.
When Should You Contact Your Doctor After Arthroplasty?
It’s important to know when to contact your doctor after surgery. Reach out if you experience:
- Bleeding
- Signs of infection, such as fever, severe swelling, or discharge from the incision
- Severe pain that does not respond to pain medication
Regain Your Mobility with Arthroplasty!
Many people regain mobility and enjoy a more active lifestyle after joint replacement surgery. However, everyone’s recovery process and timeline are different. You may need to adjust some activities to protect your new joint. Open communication with your doctor about what to expect before and after surgery is crucial. Following your physical therapy program and adhering to your orthopedic surgeon’s instructions will help you achieve the best outcome.